 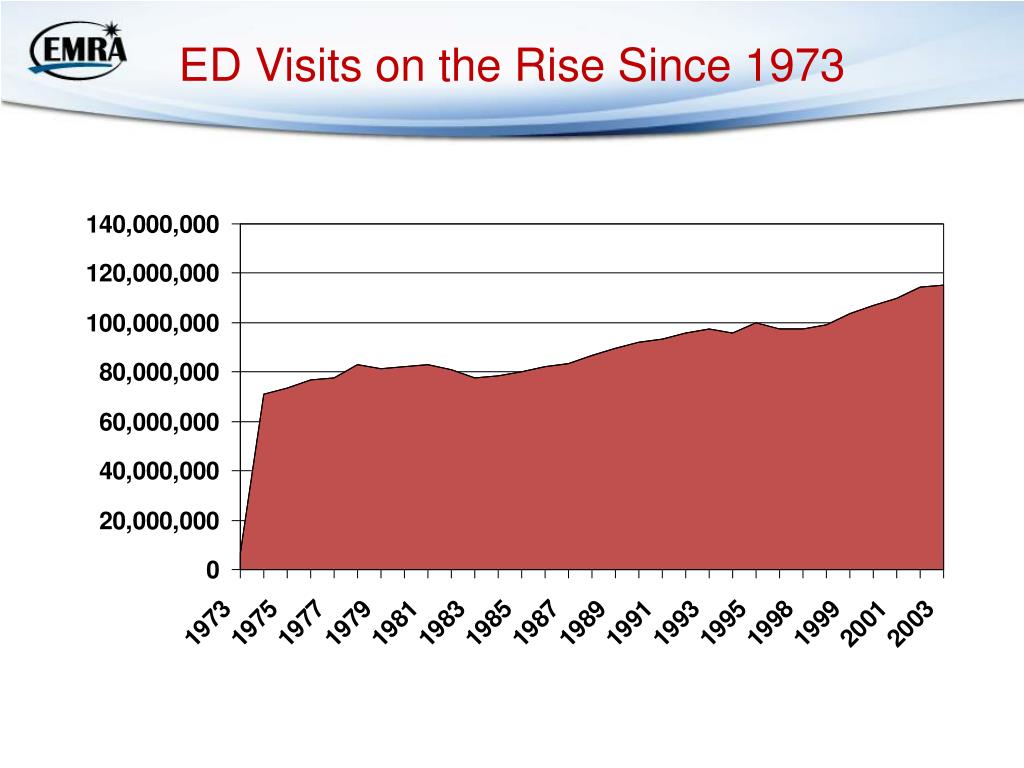
One study found that approximately one-third of individuals who presented to the ED with NCCP and who were ultimately diagnosed with PD received treatment for the PD ( 15). Several studies have provided evidence of the underuse of effective management for anxiety disorders ( 6, 13, 14) in the ED. These costs could be attenuated with timely and appropriate care within the mental health care system for those diagnosed as having anxiety disorders. It is estimated that annual health care costs for anxiety disorders reach $42.3 billion ( 12). People with anxiety disorders tend to be high utilizers of health care and place a strain on the health care system. Left untreated, anxiety disorders can result in the use of expensive ED visits, exacerbating the economic burden that mental health care places on the health care system. It is clear that effective management strategies for anxiety disorders are needed, within both primary care and emergency care. One study found that 50% of patients with panic disorder sought treatment at the ED on six or more occasions, with the first ED visit recurrence within seven days in 16.6% of the cases ( 11). ED evaluations and management are expensive, and patients with anxiety disorders tend to present for multiple ED visits ( 9, 10). Several studies have documented that panic disorder is the most common reason for seeking treatment for noncardiac chest pain (NCCP) at the ED ( 4– 8). The most common anxiety disorders are generalized anxiety disorder and panic disorder. Possibly because anxiety is associated with acute somatic symptomology, anxiety disorders are frequently treated in the emergency department (ED) as well as in primary care or mental health care settings ( 2, 3). prevalence studies estimate that anxiety disorders affect 15.7 million people each year and 30 million people at some point in their lives ( 2). population, with an estimated 12-month and lifetime prevalence of 19% and 31%, respectively ( 1). Webinar: How’s America’s Oral Health? Barriers to Care, Common Problems, and Ongoing Inequity, a webinar recording that explores the State of Oral Health Equity in America 2022 survey with three researchers and a leading oral health advocate.Anxiety disorders are the most common class of mental disorders in the U.S. 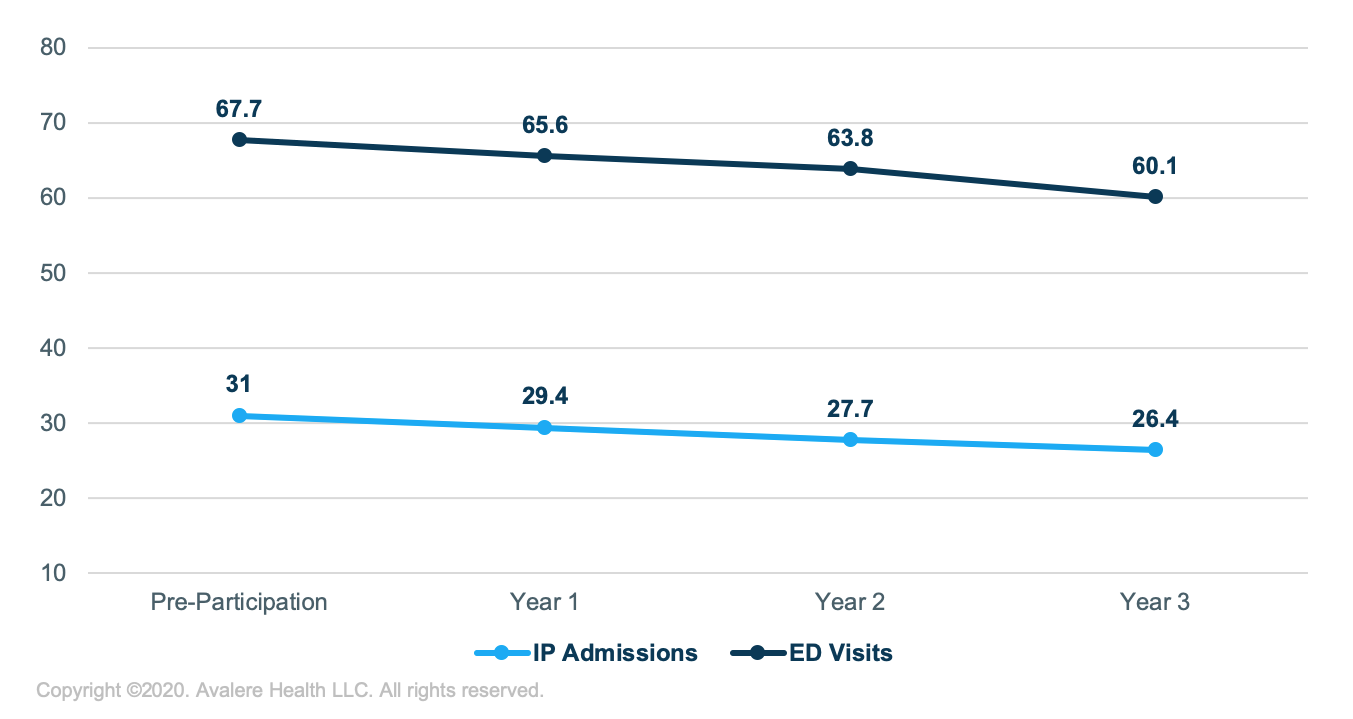
Americans Are Still Not Getting the Dental Care They Need, the first in a series of reports from our annual State of Oral Health Equity in America 2022 survey, this publication explores persistent inequities in the nation’s oral health.A Systematic Review of Dental-Related Emergency Department Visits Among Medicaid Beneficiaries, an article in the Journal of Public Health Dentistry takes an in-depth look at the incidence of dental-related ED visits for Medicaid enrollees compared to those with other types of insurance.These trends reflect changes and growing inequities in Americans’ access to dental care. Black individuals were 44% more likely to visit an ED for NTDCs compared with white individuals.Patients most likely to visit the ED for an NTDC are 25-34 years old, uninsured or have Medicaid coverage, live in a rural area, or have an income below $48,000 per year.Since 2014, average annual charges associated with ED visits for NTDCs have increased by 62%, while the rate of ED visits for NTDCs has continued to decrease.In this publication, an update from a 2020 report, CareQuest Institute researchers found: Moreover, most hospitals lack the ability to provide appropriate care for NTDCs, and the typical cost of such ED visits is much higher than a patient receiving care from a dental provider. Hospital ED visits for NTDCs can divert critical resources and create added stress for ED personnel. An updated visual report from CareQuest Institute finds that in 2019, there were 1.8 million hospital emergency department (ED) visits for non-traumatic dental conditions (NTDCs), which cost $3.4 billion to treat. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
